No formal diagnostic criteria for UFS have been published.
As is common with many genetic conditions, children and adults with UFS can have a range of symptoms and features. Most affected individuals are diagnosed in early childhood having suffered from recurrent urinary tract infection. Very mildly affected people may only be diagnosed following testing after the diagnosis of a relative. These urinary dysfunctions combined with the characteristic “inverted” facial expression can provide strong indication for the disease.
Two causative genes have been identified, the HPSE2 gene and the LRIG2 gene. Changes in these genes (mutations or pathogenic variants) are known to cause UFS. Some individuals with UFS may not have mutations in either gene.
In infancy and later childhood, bladder dysfunction that is characteristic of UFS includes: poor urinary stream and dribbling incontinence; incomplete bladder emptying can lead to urinary infection with progressive kidney failure.
Clinical Diagnosis
The clinical diagnosis of UFS can be established in an individual with urinary tract dysfunction and characteristic facial movement with expression, or the molecular diagnosis can be established in an individual with characteristic features.
Most affected individuals present to nephrology with frequent urinary tract infections during childhood. A nephrologist or urologist could diagnose the condition on the basis of the following clinical signs in combination with the characteristic facial expression.
UFS should be suspected in individuals with the following clinical findings and family history.
Classic clinical findings:
- Urinary bladder dysfunction (also termed non-neurogenic neurogenic voiding dysfunction, occult or subclinical neuropathic bladder) with detrusor overactivity and detrusor sphincter dyssynergia. Affected individuals are at risk for urinary incontinence, urosepsis, and progressive kidney failure. Urinary tract features have been present in nearly all reported individuals.
Characteristic urinary tract abnormalities:
- Prenatal ultrasonography in the second or third trimester can show an enlarged bladder (megacystis) and dilated upper urinary tracts (hydronephrosis).
- Postnatal imaging by ultrasonography and micturating cystourethrography typically shows muscular thickening and trabeculation of the urinary bladder, but appearances may also be normal.
- Hydroureteronephrosis associated with vesicoureteral reflux is common in UFS.
- Micturating cystourethrography and direct visualization by cystoscopy reveals a patent urethra, critically distinguishing UFS from conditions such as posterior urethral valves, which are characterized by an anatomic obstruction within the lumen of the urethra.
- Urodynamics is generally only available in specialist pediatric urology centers. If performed, typical findings are abnormally high hydrostatic pressure within the bladder that persists during cycles of incomplete voiding. This is associated with failure of the outflow tract to fully dilate during voiding, the so-called dyssynergic voiding.
- A characteristic abnormality of facial movement with expression, resulting from abnormal co-contraction of the corners of the mouth and eyes, which is most obvious during smiling or laughing and often described as a “grimace” [Ochoa 2004, Aydogdu et al 2010, Ganesan & Thomas 2011]. Typical facial expressions have been present in nearly all affected individuals.
Genetic Testing for UFS
Molecular genetic testing can confirm a diagnosis of urofacial syndrome. Molecular genetic testing can detect pathogenic variants in the disease specific genes (i.e., HPSE2 or LRIG2) known to cause the disorder, but is available only as a diagnostic service at specialized laboratories.
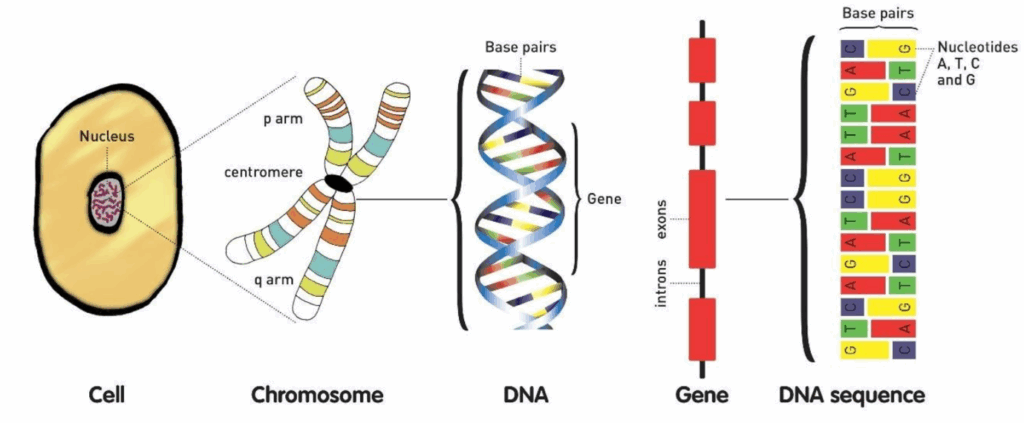
Genes are instructions that have important roles in our growth and development. They are made of DNA and are incorporated into organised structures called chromosomes. Chromosomes therefore contain our genetic information. Chromosomes are located inside our cells, the building blocks of our bodies. In people with genetic conditions, one or more of their genes don’t instruct the body as we would expect, which can lead to changes in how their body works.

~64% of individuals with UFS have changes in HPSE2 while ~20% have changes in LRIG2.
UFS has been found to be caused by specific changes (known as pathogenic variants) to the DNA sequence of either the HPSE2 gene or, less commonly, the LRIG2 gene. • The HPSE2 gene is located in the long ‘q’ arm of chromosome 10 in a region called 10q24.2 (as shown in the image to the left).
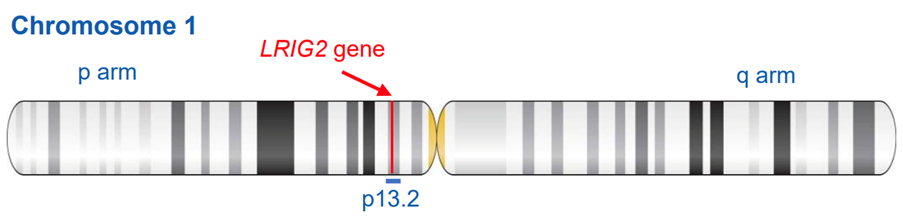
The LRIG2 gene is located in the short ‘p’ arm of chromosome 1 in a region called 1p13.2 (as shown in the image to the left).
We have two copies of chromosomes 1 and 10 in our cells, so we also have two copies of the HPSE2 and LRIG2 genes.
UFS occurs when both copies of either the HPSE2 gene or the LRIG2 gene are affected. This is known as autosomal recessive since all numbered chromosomes are called autosomes and genetic conditions that only occur when both copies of an autosomal gene are affected are known as recessive. Unique publishes separate guides to Autosomal Recessive Single Gene Disorders and Autosomal Recessive Inheritance.
The HPSE2 gene sequence is used to make a protein called heparanase 2. This protein is important because it is found in certain nerves that send instructions to parts of the body, including the bladder to control how it works.
The LRIG2 gene sequence is used to make a transmembrane protein containing leucine-rich repeats and immunoglobulin-like domains. This protein is important because, like heparanase 2, it is found in nerves that send instructions to the bladder to control how it works.
Genetic Report
The results of genetic (genomic) testing are likely to be given to you by your geneticist, a genetic counsellor or a bladder specialist who ordered the test.
An example result of a DNA sequencing test (e.g. whole exome sequencing (WES) or whole genome sequencing (WGS)), which can identify gene variants, is shown below for the HPSE2 gene.

